What Your Blood Sugar Patterns Can Tell You
Blood sugar is often discussed as if it only matters for people with diabetes. In reality, glucose regulation influences far more than most people realize. Energy levels, cravings, weight regulation, cardiovascular risk, inflammation, gut health, and even mood are all affected by how well your body handles glucose throughout the day.
The challenge is the most routine lab testing captures only a snapshot. A fasting glucose or A1c can look “normal,” while significant blood sugar swings are happening every day in response to food, stress, sleep, or exercise. This is where Continuous Glucose Monitors (CGM’s) can be especially helpful.
What a Continuous Glucose Monitor Actually Measures
A CGM is a small wearable sensor that tracks glucose levels continuously, day and night. Unlike finger-stick testing, which requires a blood sample at a single moment, CGMs measure glucose in the interstitial fluid just beneath the skin. this closely reflects blood glucose levels and allows us to see trends.
Once placed, the sensor automatically measures glucose every few minutes and transmits the data to a phone or reader. most sensors are worn for 10 to 14 days, during which time the patients continue living their normal lives, this is the key. CGMs are most useful when they capture real life, not a controlled or overly restricted version of it
Why Looking at Patterns Matters More Than Single Numbers
Traditional blood sugar tests give us isolated data points. CGMs show us pattens. Over just a few days, people often notice trends that they never expected, such as:
Sharp spikes after certainmeals
Higher readings during stress or poor sleep
Morning elevations related to cortisol
Drops after intense exercise
This allows us to move beyond generic advice and toward something far more useful: understanding how your body responds in your context.
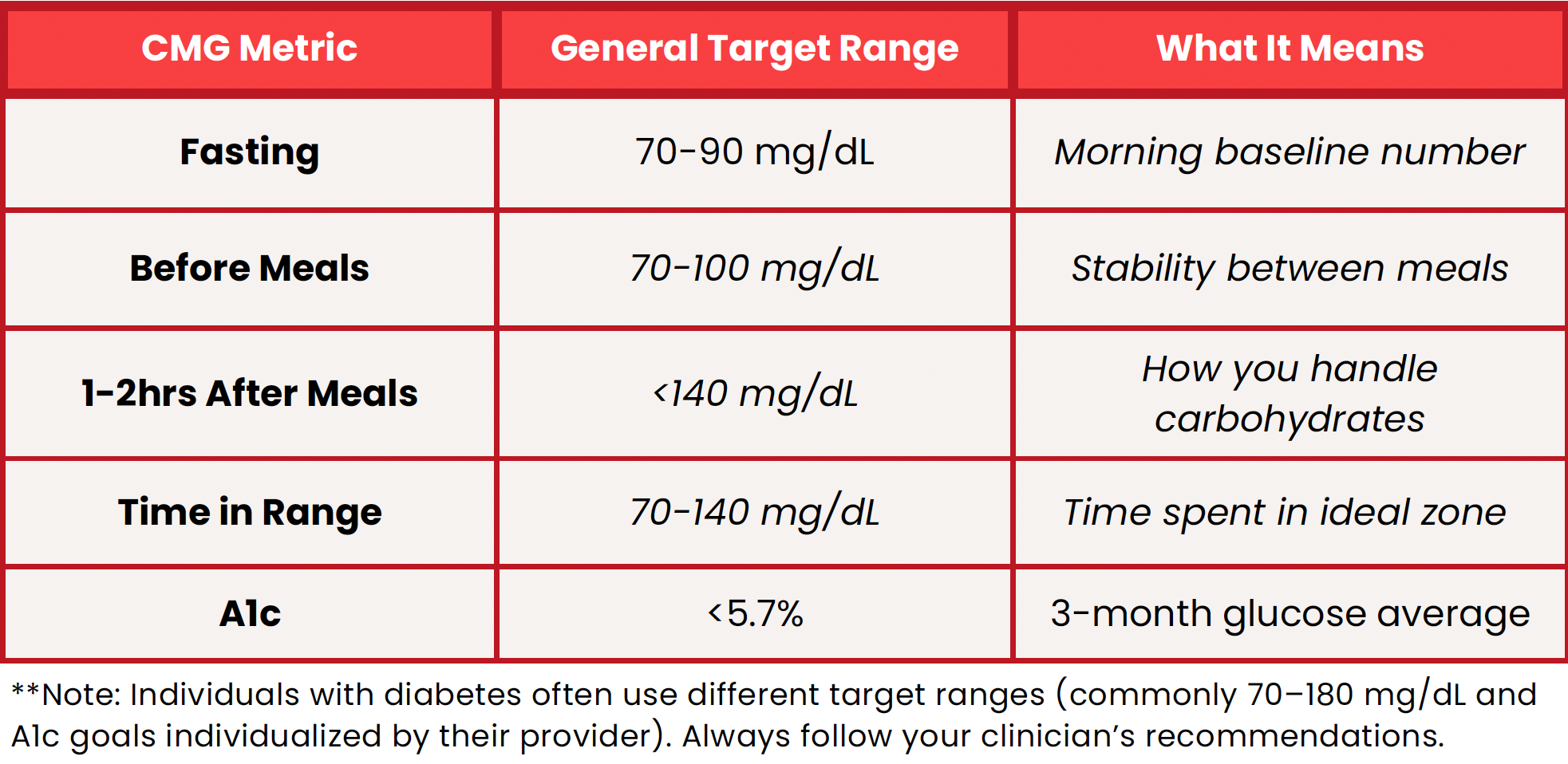
What We Look for in Healthy Glucose Regulation
In preventative and functional medicine, we care less about perfection and more about stability.
In general, we look for:
A relatively steady fasting glucose
modest rises after meals
a return toward baseline within 1-2 hours
fewer large swings throughout the day
Large, frequent glucose fluctuations place repeated stress on insulin and are associated with inflammation, insulin resistance, vascular damage, and increased cardiometabolic risk over time. CGM’s often reveal early dysfunction long before it shows up on routine labs.
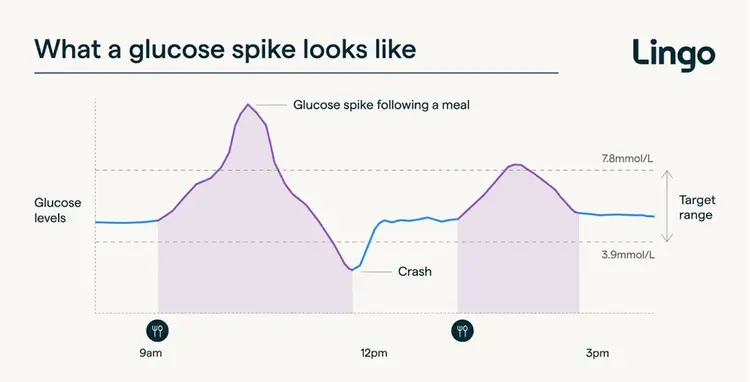
Why Blood Sugar Spikes Matter
When glucose rises quickly after eating, the body releases a large amount of insulin to bring it down. That rapid drop often leads to fatigue or brain-fog, hunger shortly after eating, cravings for quick carbohydrates.
Repeated spikes are not just uncomfortable. Over time, they contribute to oxidative stress, inflammation, strain on the pancreas, and disruption of the gut microbiome. The goal is not to eliminate glucose rises entirly, but to create smaller, smoother rises that resolve efficiently.
Using CGM as a Learning Tool
When we use CGMs clinically, we often recommend a two-week approach.
Week one is about observation. Patients eat normally and simply notice how meals, sleep, stress, and activity affect their glucose.
Week two is about gentle experimentation. small changes often make a noticeable difference, such as:
Adjust meal timing
Changing food combinations
Modifying portion sizes
Paying attention to food order
Because the feedback is immediate, patients can see what works for their body rather than guessing.
Why the Order You Eat Food Matters
One of the simplest strategies we see work consistently is food order.
Eating vegetables, protein or healthy fats before carbohydrates can significantly reduce post-meal glucose spikes. Fiber slows absorption, and protein and fat further moderate the clucose response.
A simple way tho think about it:
Start with vegatbles or salad
move on to protein and healthy fats
finish with carbohydtates
This approach has been used as medical nutrition therapy in countries like Japan and works well for people with and without diabetes.
Resistant Starch and Glucose Stability
Another pattern CGMs often reveal involves resistant starch. When foods like rice, potatoes, or pasta are cooked and then cooled, part of the starch becomes resistant to digestion.
This can slow glucose absorption, reduce post-meal spikes, and support gut health. Cold versions tend to have the strongest effect, though even reheated starches usually preform better than freshly cooked ones.
Timing Matters: Late-Night Eating
CGMs frequently show higher overnight glucose or elevated fasting glucose after late or heavy evening meals. this reflects the natural slowing of metabolism as the day winds down.
When possible, finishing dinner earlier, often around 6 - 7 pm, supports better overnight glucose regulation and aligns more closely with circadian rhythms than simply counting hours before bed.
Blood Sugar Is Influenced by More Than Food
One of the most important lessons CGMs teach is that glucose is affected by far more than diet alone. Common influences include:
Stress and anxiety
Poor sleep
Illness or inflammation
Hormonal shifts or pain
Dehydration
Caffeine or alcohol
Certain medications
Artificial sweeteners (in some people)
Gut imbalance
Seeing these patterns help reduce frustration and unnecesary restricion, and allows for more thoughtful compassionate adjustments.
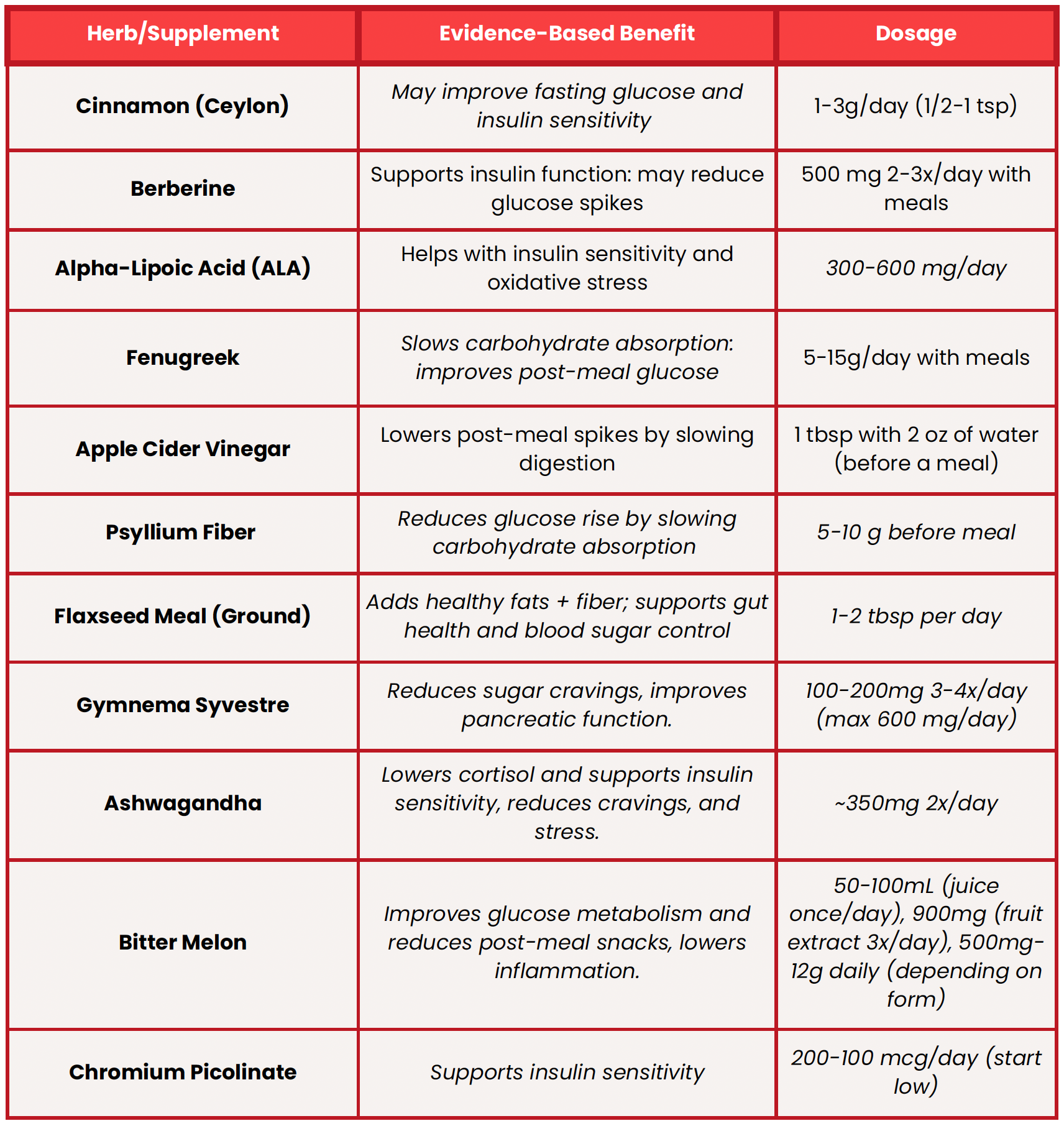
Supporting Blood Sugar Naturally
Always talk to your healthcare provider before starting any supplement, especially if you take medications.
The Gut-Glucose Connection
Blood sugar regulation and gut health are closely linked. Diets high in refined sugars can disrupt the microbiome and increase inflammation. In contrast, balanced glucose supports microbial diversity, immune regulation, and cardiovascular health.
A healthy gut supports stable blood sugar - and stable blood sugar supports a healthier gut!
The Bigger Picture
A CGM is not a test to pass or fail. It is a tool for awareness.
By understanding how your body responds to daily life, you can make small, informed changes that support long-term metabolic and cardiovascular health. For many people this insight is far more powerful than generic advice.
At Gutwell Medical, CGMs are one piece of a broader functional approach focused on education, personalization, and prevention - not restriction or fear.